Grade 3 Varicocele: Do You Really Need Surgery?
Fertility Treatment
Varicocele is one of the most common testicular conditions that enlarge the veins above the testes (in the scrotum) and varicose. These veins are called the pampiniform plexus. Varicocele is categorized into three grades, with grade 3 being the most severe and painful.
In grade 3 varicoceles, testicular pain worsens with exercise and prolonged sitting or standing. If the grade 3 varicocele is not treated correctly, it may lead to complications such as testicular atrophy (the shrinking of the testicles) and male infertility.
What Are the Grades of Varicocele?
There are 3 grades of varicocele ranging from mild to severe as follows:
- Subclinical varicocele (Grade 0): a varicocele that is not detectable merely by physical exam, and its diagnosis requires an ultrasound;
- Grade 1 varicocele: a mild varicocele in which the veins above the testicles are palpable by pressing the abdomen;
- Grade 2 varicocele: a moderate varicocele in which the testicular veins are only palpated in a standing position;
- Grade 3 varicocele: the most severe varicocele in which the veins in the scrotum are easily visible while standing.

What Is a Grade-3 Varicocele?
A grade 3 varicocele, the most severe type, causes severe testicular pain. In a grade 3 varicocele, the testicular veins are easily visible. Different types of Varicocele occur in 10-15% of men and will cause male infertility. By creating obstruction and scrotal swelling, the varicocele condition raises the testicular temperature and will result in sperm damage.
A grade 3 varicocele may develop even at a young age and sometimes need no special treatment. However, in most cases, the patients should undergo treatments like surgery as soon as possible.
What Are the Symptoms of Grade-3 Varicocele?
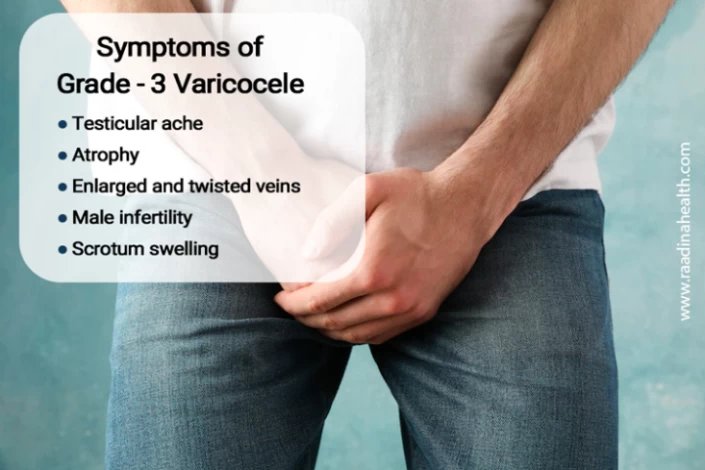
The most common signs of grade-3 varicocele are as follows.
- Testicular ache, especially while standing and during physical activities;
- Painless testicular lumps and scrotal swellings;
- Atrophy or the shrinking of the testicle;
- Enlarged and twisted veins within the scrotum;
- Male infertility in adults;
- Scrotum swelling;
- Decreased testicular size in children;
- Severe and continuous discomfort that worsens as the day goes on;
- Pain relief when lying on the back.
What Are the Causes of Grade-3 Varicocele?
Grade 3 Varicocele is correlated with the condition of the testicular blood veins. The testes are connected to the spermatic cord. Each cord contains veins and nerves that support the vascular veins.
Healthy veins within the scrotum continuously transport blood from the testicles to the scrotum and the heart. However, in some cases, the normal flow is disrupted by spermatic cord vessels, and blood backs up in the veins, which makes the veins enlarged. This condition, left-sided grade 3 varicocele, often occurs in the left testicle and causes testicular damage and male-factor infertility.
Is Grade 3 Varicocele Dangerous?
A grade 3 varicocele is not fatal. However, it can rarely be associated with dangerous conditions. Right-sided varicoceles may indicate a blockage in the abdomen. These obstructions can result from blood clots, tumors, or internal organ problems. Also, in rare cases, varicoceles could lead to dangerously low testosterone levels, resulting in metabolic syndrome, diabetes, and osteoporosis.
What Are the Risks and Complications of Grade 3 Varicocele?
- Testicular Damage
- Infertility
- Decreased testosterone levels
- Pain
Testicular Damage
Testicular damage is a gradual process that prevents the proper growth of the testicles and will worsen over time. Sometimes, a unilateral varicocele may cause one testicle to grow less than the other. Delayed treatment of grade 3 varicocele may help balance the production of hormones and sex cells but cannot return the testes to their standard size.
Infertility
Grade 2 and 3 varicoceles affect male fertility by reducing the number and quality of sperm. 40% of infertile men with primary infertility have varicoceles. This condition is also observed in 80% of men with secondary infertility (men who cannot conceive a second child).
Decreased testosterone levels
Varicoceles might cause low testosterone levels. The Grade 3 varicocele may damage the cells that produce testosterone hormone, disrupt testosterone function, and affect secondary male characteristics such as tone of vocal change, generating muscle mass, body hair, libido, etc.
It should be noted that testosterone levels may increase by 100ng/dL in many men after varicocele surgery (varicocelectomy).
Pain
Other symptoms of grade-3 varicocele include scrotal pain, discomfort, or a feeling of heaviness and tension in the testicles. These signs often worsen while standing and lifting or pulling objects. Scrotal pain may continue in 50% of men after surgical treatment.

How Does a Grade 3 Varicocele Cause Infertility?
As mentioned above, varicocele is one of the most common causes of male infertility. Increased testicular temperature causes fundamental changes in the body and will lead to the two below disorders in sperm production:
- First, the increased testicular temperature caused by decreased testosterone level leads to complications such as low sperm count (oligoasthenoteratozoospermia), poor sperm motility and morphology, and reduced sperm fertilizing power;
- Second, the elevated testicular temperature may cause chemical changes and sperm DNA damage, hurting the sperm's outer layer (membrane) and health.
The production of sufficient and high-quality sperm depends on the testicular temperature. Normally, the testicular temperature should be 2 to 3C lower than the core body temperature. However, due to blood failure to leave the testis in varicocele, the testicular temperature rises higher than the normal level and disrupts the process of sperm production.
On the other hand, varicoceles cause less oxygen and more waste products in the testis veins, leading to testicular damage and spermatogenesis disorders.

How to Diagnose Grade 3 Varicocele?
A healthcare provider might perform a physical examination or recommend a scrotal ultrasound to diagnose varicose veins. The severity of the condition is then measured according to varicocele grading as 1, 2, or 3.
There are several methods to diagnose varicocele, as follows:
- Physical examination
- Doppler Stethoscope
- Ultrasound
Physical examination
The grade 3 varicocele usually shows more obvious symptoms and is easily detectable through physical examination. However, the final diagnosis requires additional tests.
In a grade 3 varicocele, the doctor performs a routine physical exam to check the appearance of the testicles. This type of varicocele is large enough that a mass like a "bag of worms" may be visible above the testicle. The urologist also performs the Valsalva maneuver. This technique asks the patient to take a deep breath while standing and holding it. Valsalva maneuver helps find the enlarged veins by touching the skin of the scrotum.

Doppler Stethoscope
The doctor can also diagnose a grade 3 varicocele using a stethoscope. In this method (Doppler Stethoscope), the doctor merely listens to the pumping sound of the blood artery that passes by the testicle as the patient lies in a relaxed position. The blood flow in the veins is very slow, and no sound can be heard. However, if the patient pushes down his abdomen, more blood will flow into the scrotum, and a rushing sound will be heard.
Ultrasound
Ultrasound is the most accurate non-invasive method to diagnose varicoceles. It consists of two steps:
First, an ultrasound imaging of the scrotum is performed to measure the diameter of the veins and identify other abnormalities. One-third of infertile men normally diagnosed in the physical examination show abnormal results in the ultrasound.
The second step is to measure the amount of blood flow passing through the probe while pushing down the abdomen. The doctor will check the sound or color image of the testicles and determine whether varicocele exists.
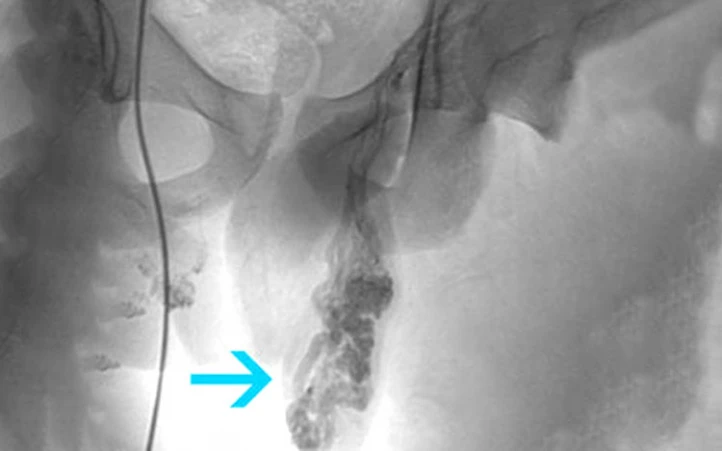
Generally, ultrasound imaging uses sound waves to record pictures of the inside of the body. Varicoceles signs on the ultrasound are more than 3 mm diameter veins and abnormal blood flow. The ultrasound test can also show the size of the testicles.
The doctor may also recommend additional tests, such as a sperm test, to ensure the testis function.
Grade 3 Varicocele Treatments
The main treatment options for grade-3 varicocele include open surgery, laparoscopic, and subcutaneous embolization. Choosing each procedure depends on factors like the severity of varicocele, the condition's symptoms and complications, and the patient's decision to have children.
Sometimes, the patient with grade 3 varicocele can have children without treating the disease. However, if the patient is experiencing pain, infertility, and testicular weakness, he must undergo suitable treatment.

Varicocelectomy improves testicular veins and blood flow and will increase the number and quality of sperm. Varicocele treatment, especially in teenagers, aims to cure severe and continuous pain, advanced testicular atrophy, and abnormal sperm production.
In the following, we will introduce and review several ways to treat varicocele grade 3:
- Varicocelectomy
- Laparoscopic varicocelectomy
- Percutaneous Varicocele Embolization
- Microsurgical Subinguinal Varicocelectomy
- Inguinal Varicocelectomy
- Retroperitoneal Varicocelectomy
Varicocelectomy
Varicocelectomy, also known as varicocele repair, is the most common treatment for grade 3 varicocele. This microscopic surgical technique gives the doctor a better view of the affected area and is often performed under local anesthesia.
During varicocelectomy, the surgeon makes an incision to access the scrotum and find the enlarged veins. Then, the doctor cuts any enlarged veins that are blocking blood flow. Using a microscope increases the accuracy of the surgery and helps the doctor see ductus deferens, testicular arteries, and veins.
Since any damage to the vascular arteries and diaphragms affects sperm and testicular health, the expertise and precision of the surgeon are essential factors in varicocelectomy.
Laparoscopic varicocelectomy
Laparoscopic varicocelectomy is done under general anesthesia. It uses an intra-bladder catheter to drain urine and prevent surgery disruption. First, the doctor makes a small incision under the belly (abdomen) and fills the abdomen with gas. A video camera is then placed inside the abdomen with a surgical tool. Two additional incisions are also made in the abdominal wall to place working tools. This makes space for the surgeon to see the location of enlarged veins and work. When the surgery is done, the incisions are closed with stitches.
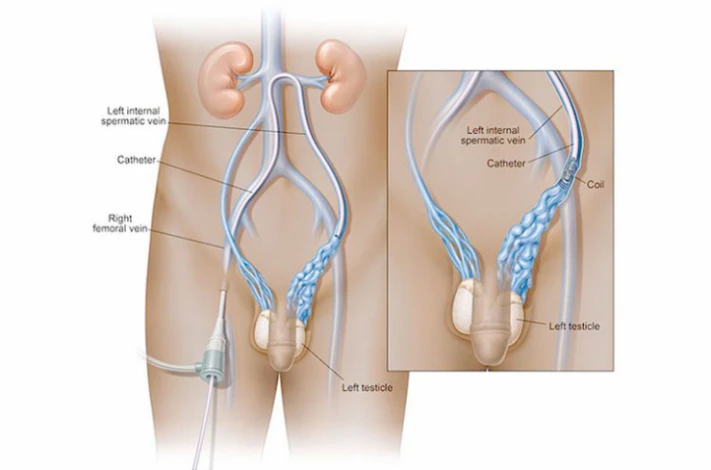
Percutaneous Varicocele Embolization (Varicocele Treatment without Surgery)
In the percutaneous embolization procedure, a small incision is made in the groin, and a long catheter tube is inserted into the leg vein. X-rays will help the healthcare provider move the tube to the location of the most prominent vein of the body (Vena Cava). Then, the doctor will release a blocking agent into the affected veins. It usually reroutes blood flow into other nearby veins. Although the vein blockage is sometimes bypassed from the capillary paths, it is impossible to block the area entirely and prevent the spread of the disease with this method.
Inguinal Varicocelectomy
An incision is made in the lower abdomen and below the navel in inguinal varicocelectomy. Then, the affected veins are cut using a magnifying lens or even with the naked eye. This cut is in a higher location, larger than a sub-inguinal cut, and its scar can be seen. The post-surgery pain and the recovery time will also be more due to the abdominal incision.
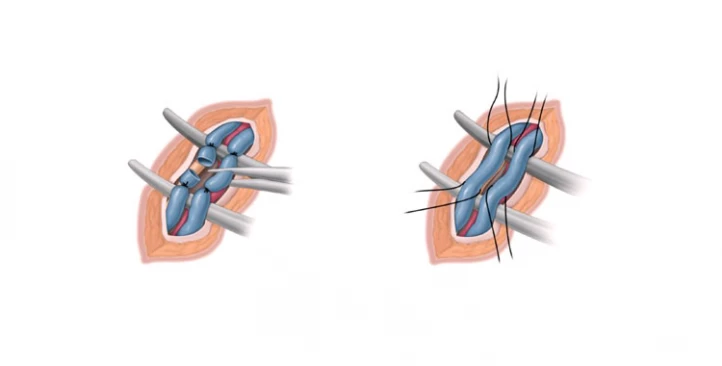
Retroperitoneal Varicocelectomy
In retroperitoneal varicocelectomy, a higher incision is made to cut off the veins and the abdominal incision. The incision scar is apparent, and the post-surgery pain and recovery time are high due to the abdominal incision. The probability of treatment failure in the retroperitoneal varicocelectomy method is 15-25%, and the risk of hydrocele is about 7%.
Microsurgical Subinguinal Varicocelectomy
During microsurgical subinguinal varicocelectomy, one or two incisions are made above the penis. The incisions allow the doctor to access the spermatic cord (which contains veins, vessels, muscles, and lymph that support the testicle). The post-surgery pain, discomfort, and recovery time are less since no incision is made on the abdomen in this procedure.
Furthermore, a microscope provides a clear view of all veins and reduces the risk of damage to veins and lymph vessels.
Grade-3 Varicocele Surgery Aftercare
Although microscopic varicocele surgery is an easy outpatient surgery with a high recovery rate, taking only an hour, some measures and aftercare tips should be taken to reduce pain and possible side effects and increase varicocele surgery recovery speed.
- Take pain relievers under the doctor's supervision;
- Walk to prevent blood clots;
- Return to work after one day (for sedentary jobs);
- Avoid exercise for 10 to 14 days;
- Avoid heavy activities;
- Avoid heavy lifting for 2 weeks;
- Rest Adequately;
- Visit the doctor regularly and follow up on the surgery results with an ultrasound.

Varicocele Grade 3 Natural Treatment
Natural treatments may be supplementary to medical options and should not be considered the only solution. These therapies include:
- Have a healthy diet and increase the intake of fiber-rich foods such as fresh vegetables, fruits, and whole grains;
- Do Kegel exercises to improve and restore blood flow;
- Consume herbal medicine after a consult with a health provider;
- Wear jockstraps for proper scrotal support;
- Use ice packs and cold compressions to get relief from the testicular swelling;
- Do Yoga to improve blood circulation;
- Increase the intake of antioxidants;
- Stay at a stable weight and make a lifestyle change.
Azoospermia and Grade 3 Varicocele
Azoospermia is one of the relatively common male conditions when male genital organs produce no sperm. Studies show that in some cases, varicocele treatment has improved azoospermia as well. In other words, surgery can increase fertility and the chance of natural pregnancy in 50% of men with azoospermia, up to 3 times compared to other treatments.
The characteristics and genetic problems of patients with azoospermia should be evaluated before performing varicocelectomy to identify the cause of the problem. In case of a lack of sperm production due to hereditary disorders, surgery will not be a good solution. Measuring some factors, such as the degree of varicocele, testicle size, body hormone levels, and test parameters, helps the doctor make better decisions about choosing a proper treatment.
Hydrocele vs Varicocele
In a normal situation, a small amount of lubricating fluid is continuously produced inside the scrotum to allow the testis to move freely. The veins in the scrotum usually drain away excess fluid. Testicular hydrocele occurs when this process fails, and fluid accumulates inside the scrotum.
If the patient suffers from varicocele and the swollen testicular veins are not completely treated by surgery, or he does not rest enough after the surgery, the fluid may collect around the testicle and cause hydrocele. In such cases, if the fluid around the testicle is low, the condition does not need any treatment and will be cured per se; however, the best way to treat swollen and enlarged veins is to drain the fluid around the testicle.

When to see a doctor?
Patients should see a doctor when they experience varicocele symptoms for a timely and accurate diagnosis. These symptoms include a change in the size, shape, and appearance of the testicle, a lump or swelling in the testicular area, the feeling of abnormally large or twisted veins inside the testicle, and infertility.
Conclusion
Varicocelectomy in Iran can be done under the supervision of highly experienced Iranian physicians and surgeons. The cost of grade 3 varicocele surgery in Iran varies depending on the severity of the condition, the type of surgery, the facilities of the hospital, and the surgeon's fee. The average cost of varicocelectomy in Iran is from $1,300 to $4,500.
For more information about the cost of varicocelectomy in Iran and to schedule an appointment in advance, you can contact our team at Raadina Health.
We are linked with the most equipped hospitals and specialists, facilitating your treatment process in Iran. We also provide you with pre-arrival consultations and help to learn about the most appropriate treatment for your problem. For a free consultation and personalized guidance, call the expert advisors at Raadina health tourism company .

FAQ
What are the varicocele grade 3 effects?
The effects of Grade 3 varicocele can be significant, especially regarding reproductive health. The severity of the condition in linked to decreased sperm production and quality, which may lead to male infertility. Moreover, it can cause discomfort, pain, and potential testicular atrophy if left untreated.
How big is grade 3 varicocele?
Grade 3 varicocele size is large, characterized by palpable veins in the scrotum that are easily visible. The size of these veins is typically more pronounced than in lower grades.
What are the risks of not treating Grade 3 varicocele?
Untreated Grade 3 varicocele can lead to complications such as male infertility, testicular shrinkage, and chronic pain.
Will Grade 3 varicocele treatment improve my fertility?
Many patients experience improved fertility after treatment for Grade 3 varicocele, particularly if they were experiencing male infertility related to the condition. However, results may vary, and it's important to have realistic expectations.
Is grade 3 varicocele treatment without surgery possible?
While pain relievers, scrotal support, and lifestyle changes such as weight management, avoiding prolonged standing or heavy lifting, and wearing supportive undergarments can temporarily relieve symptoms, surgery remains the most effective and permanent treatment for Grade 3 varicocele, particularly when male fertility is a concern.
Can testicular varicocele be treated without surgery?
Yes, mild to moderate varicoceles can sometimes be managed without surgery. Supportive measures like wearing supportive underwear, lifestyle changes, weight management, and anti-inflammatory medications may help reduce pain and swelling. However, for severe cases affecting fertility, surgery is usually more effective.
What are natural treatments for varicocele without surgery?
Light exercises such as walking and aerobic workouts, anti-inflammatory foods, avoiding prolonged standing or sitting, and wearing supportive underwear can help improve blood circulation and reduce symptoms. Keep in mind that these methods cannot completely resolve severe varicoceles.
Can lifestyle changes really improve varicocele?
Yes, lifestyle improvements can help reduce discomfort and improve sperm quality, particularly in mild to moderate cases. However, grade 3 varicoceles usually require medical or surgical intervention for full management.










User
-Thank you very much for your help and all detail information. May God be with you.