What are the Main Causes of Varicocele?
Fertility Treatment
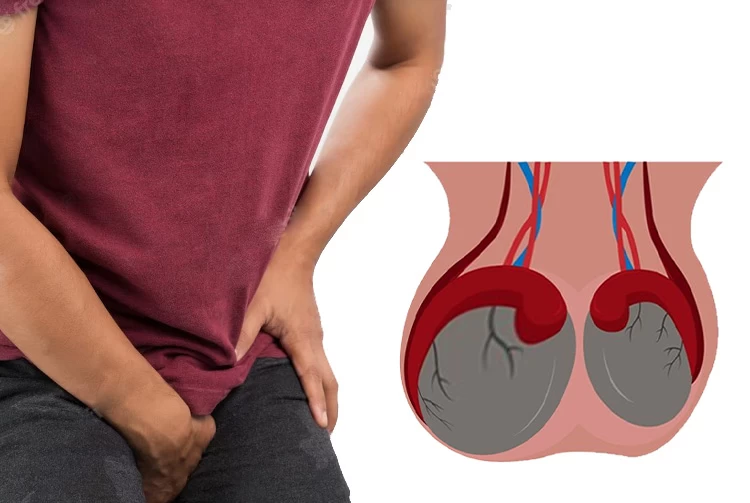
One of the most common causes of male infertility is the abnormal enlargement of the veins above the testicles, commonly known as varicocele. In a varicocele, the veins of the scrotum swell and cause pain and discomfort. Also, by shrinking the size of the testicles, varicocele decreases the quantity and quality of sperm, reduces testosterone production, and may cause male infertility.
Varicocele does not directly cause sexual dysfunction or premature ejaculation but can cause serious problems, such as reducing sperm motility and changing shape. Fortunately, even though 20-30% of young men suffer from varicocele, most get treated with modern varicocelectomy treatment methods.
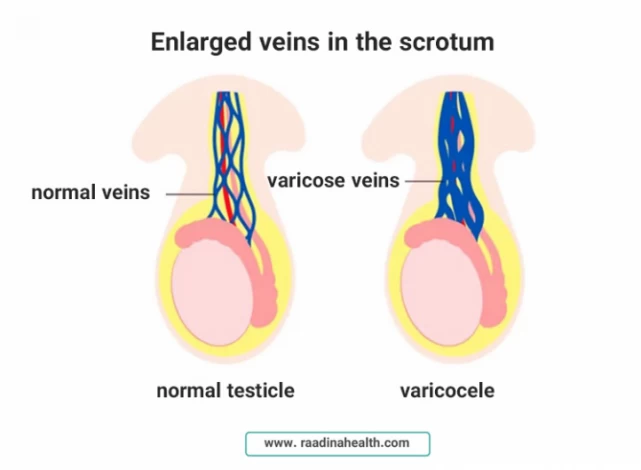
Types of Varicocele
In a varicocele, the veins do not transfer oxygen-depleted blood from the testicles to the kidney, so the blood remains around the testicle and causes discomfort. In general, varicocele is divided into three categories based on its severity: grade 1 (mild), grade 2 (moderate), and grade 3 (severe).
Varicocele grade 1
Grade 1 varicocele is a common type often diagnosed by color Doppler ultrasound. After the initial preparation of the patient, the doctor performs periodical examinations on him to find the varicocele vein.
Varicocele grade 2
In grade 2, the doctor may diagnose the disease after examining the scrotum. Also, an examination can quickly diagnose moderate varicocele when the patient lies down.
Varicocele grade 3
Severe varicocele is like a bag of twisted veins and can only be treated surgically. Also, varicocele grade 3 can easily be seen by the naked eye.
Varicocele Signs and Symptoms
Varicocele has no specific symptoms and can only be identified by examining the scrotum veins. If your veins enlarge while standing, you probably have varicocele grade 1, and if the swelling of the vessels is more prominent while you are lying down, you perhaps have varicocele grade 2. In any case, visit a urologist as soon as you notice any of the following symptoms:
- Painless swelling inside the scrotum;
- Swollen and twisted veins inside the scrotum;
- Pain in the scrotum;
- Enlargement of the testicles;
- Asymmetry of the testicles;
- Having a feeling of stretching and heaviness in the testicles and
- Not conceiving after a year of trying.

Varicocele Pain: How It Feels Like
You may wonder how varicocele’s pain feels and when and where it emerges first. In the following, the features of scrotal pain related to varicocele are mentioned:
- At first, the pain of varicocele is mild and localized and mainly starts after puberty;
- You may feel more pain on the left testicle than on the right one because 95% of varicoceles happen on the left side of the scrotum;
- You may feel pain around or above the varicocele vein, but you have no pain in your groin;
- The pain and feeling of heaviness in the scrotum increase gradually;
- The pain intensifies while standing, sitting, and doing physical activities such as sports or sex;
- You probably have more pain at the end of the day and no pain in the morning after a good night’s sleep;
- You feel less pain when you are lying down (as opposed to the persistent inflammatory pain of epididymitis); and
- The pain is not relieved by taking regular painkillers.

Causes of Varicocele
The actual causes of varicocele are not determined yet, but it mainly occurs because of several factors, such as:
- Congenital disorders: congenital problems in the testicles’ valves can cause varicocele, shrinking of the testicles, loss of sperm quality, damage to the sperm cells, and fertility disorders.
- Abdominal pressure: One of the factors that cause varicocele is abdominal pressure. This problem, caused by a retroperitoneal tumor or other diseases, provides the basis for the formation of varicocele by disrupting the blood flow inside the scrotum.
- Heavy exercise: Doing heavy exercises such as bodybuilding, weight lifting, or demanding work that puts a lot of pressure on the body can also cause varicocele if the valves of the testicles get damaged.
Varicocele Risks and Complications
Like other diseases, varicocele and its surgery have some risks and complications, such as:
- Infertility due to the reduction in sperm count and motility;
- Decrease in testosterone production;
- Testicular atrophy;
- Difficulty in urinating;
- Infection at the surgical site after varicocelectomy;
- Damage to the testicles and its artery; and
- Hydrocele (accumulation of fluid in the scrotum).
Varicocele and Male Infertility
Varicocele reduces the quantity and quality of sperm by increasing the temperature of the testis. Therefore, in many cases where the cause of male infertility is not recognized, the patient probably has an unidentified varicocele. In such conditions, varicocele can often be diagnosed while the patient is standing, but there is no sign of it when he lies down. Not all patients with varicocele have fertility problems, but many cases of male fertility disorders are related to this problem.
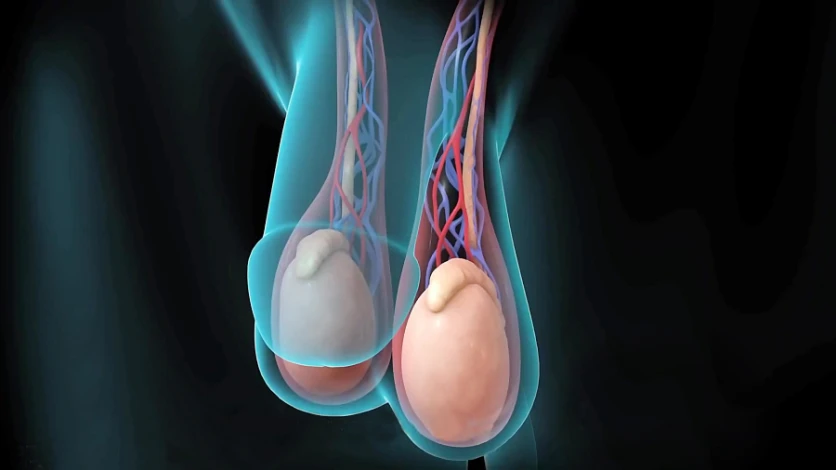
Varicocele Diagnosis
There are several steps to diagnose a varicocele, the first of which is a physical examination while standing. Then, by taking standardized tests such as ultrasound scanning of the testicles, the diameter of the vessels and the direction of the blood flow can be recorded, and the disease can be diagnosed.
We should note that in varicocele grade 1, the Valsalva maneuver can only detect veins' dilatation. In contrast, in grade 2, it can be detected by pressing the abdomen and physical examinations of the scrotum. Varicocele grade 3 is also so apparent that it can be diagnosed even with the naked eye.
In the following, two of the most common types of diagnosing varicocele are introduced:
- Physical examination
The doctor or patient can diagnose varicocele by physically examining the scrotum. During the physical examination, a mass like a bag of worms is often observed on top of the testicles. If the mass is large, the doctor can feel or touch it, but if the mass is small, the patient should take a deep breath and hold it during the Valsalva maneuver so that the doctor can detect the abnormal enlargement of the veins.

- Ultrasound examination
If the varicocele couldn't be detected by physical examination, scrotal ultrasound should be used to scan the internal structure of the scrotum. During this examination, images are recorded by high-frequency sound waves, and the varicocele symptoms are detected. In other words, the most common method of diagnosing varicocele is using color Doppler ultrasound, which shows dilated and twisted veins in gray.
By observing the dilated veins, the doctor can examine their diameter and comment on the type and severity of the disease. Of course, measuring the diameter of the veins is not definitive, but it helps identify the disease's severity.
Varicocele Treatment
Varicocele is a benign disease; varicocelectomy is the only way to treat it. Of course, as long as this disease does not have severe complications, there is no need to perform varicocele surgery. Usually, varicocelectomy is done for patients with varicocele grade 3 who wish to have children, have abnormal semen test results, have constant pain in and around the testicles, and suffer from testicle atrophy severity of the disease. The main goal of treating testicular varicocele is to redirect the blood flow in the testicular, which usually improves the quality of the sperm.
In varicocele surgery, the doctor makes a small incision on the abdomen and blocks the enlarged veins. The extent of this operation depends on various factors such as the patient's age, the disease's severity, the number of children he already has, being single or married, the association of varicocele with his sperm disorders, and his intention to have children shortly, etc.
Varicocele surgery is usually done in four ways: laparoscopy, microsurgery, open surgery, and embolization. Of course, none of these techniques is superior to the others, and the doctor chooses one based on the disease's severity. Also, in some cases, the surgical treatment of varicocele has complications such as infection, recurrent varicocele, hydrocele (accumulation of fluid in the scrotum), damage to arteries, etc.
How to Relieve Varicocele Pain?
As mentioned, mild and moderate varicocele usually don’t have apparent symptoms and are diagnosed only by physical examinations, ultrasound, and fertility tests. However, varicocele grade 3 shows more symptoms, such as severe pain, especially during physical activity and standing. This pain is sometimes vague, sharp, and distinguishable. For example, your pain may gradually intensify during the day, or your lower back may suddenly hurt when you lie on the bed.
On average, 5-10% of varicoceles are accompanied by pain. Still, they can be treated with non-invasive methods such as changing your lifestyle, not wearing tight clothes, not standing for long periods, keeping testicles cool, washing them with cold water, etc. Still, if these methods don’t work, surgical treatment is needed. In 50% of cases, the pain disappears completely after varicocelectomy; in 25-40% of cases, it is greatly reduced.
Types of Varicocele Surgery
Open surgery is the most invasive treatment for varicocele, in which a large incision is made on the groin, and the dilated veins are blocked.
Laparoscopy: In this method, done under general anesthesia, laparoscopic cameras, and surgical tools are inserted into the body through a small incision, and the damaged vein is blocked.
Embolization: This method is also performed under general anesthesia and requires the knowledge of a radiologist and a urologist. In the embolization method, a tube is inserted into the veins from the groin or neck, and a particular solution blocks the enlarged vein.
Microsurgery: It is a complicated but less-invasive method through which a small incision is made on the lower abdomen. This method inserts microscopic tools into the body to block the varicocele vein and redirect the blood flow.
Varicocelectomy Aftercare
- Avoid having food until six hours after the surgery;
- Avoid unnecessary walking and climbing until a day after the surgery;
- Avoid heavy activities for at least three days;
- You can take a shower after your bandages are removed;
- Take the prescribed antibiotics and painkillers on time;
- Avoid heavy sports for three to six months;
- In case of having a fever above 38˚ C, contact your doctor immediately and
- Go for annual check-ups.

How to Prevent Varicocele?
Varicocele is a fairly common disease that cannot be prevented in most cases. However, you can decrease its risk by considering the following tips:
- Avoid wearing tight clothes;
- Have a healthy and balanced diet to prevent constipation;
- Avoid lifting heavy objects;
- Check your BMI and blood pressure regularly;
- Stay hydrated;
- Perform check-ups every six months;
- Exercise regularly and
- Stop smoking and drinking.
conclusion
In general, varicocele is the enlargement of the scrotum’s veins, sometimes leading to male infertility. Usually, varicocele has no apparent symptoms but pain and discomfort in the testicles, so in case of any of the symptoms mentioned above, visit your urologist. There has been no drug treatment for varicocele, but it can be treated through varicocelectomy.
Raadina Co. offers the most affordable and wholesome packages of varicocele treatment in Iran if you are suffering from varicocele.
Contact us for more info on applying for an Iran medical visa, the price of different types of varicocele surgery, and the best Iranian surgeons for varicocelectomy.
Contact us for a free initial consultation about varicocelectomy
WhatsAppTelegramFacebookEmailFAQs about Varicocele
How likely is a varicocele to cause infertility?
Varicocele is one of the most common causes of infertility in men. 35% of men with primary infertility and 70 to 80% with secondary infertility suffer from varicocele.
How long does varicocele last?
Varicocele will not go away on its own and needs surgical treatment. Once the treatment is over, it takes 2 to 4 weeks for the varicocele vein to disappear.
Can varicocele be cured completely?
Although there is no definite way to prevent varicocele, it can be cured entirely by varicocele surgery. Fortunately, in most cases, the result of the varicocelectomy is permanent, and in only 2-20% of cases, the varicocele may recur.
Is exercise good for varicocele?
People with varicocele are usually advised not to do exercises such as basketball and volleyball, weight lifting, rock climbing, etc., as they worsen the pain and swelling of the damaged vein. Suppose you want to relieve your pain by exercising. In that case, you can ask your trainer to give you an exercise plan consisting of yoga poses, stretching exercises, calf raises, and walking.
What foods are good for varicocele?
Having an anti-inflammatory diet helps reduce varicocele pain and swelling. Also, foods rich in fiber, vitamins C and E, and omega-3 fatty acids are good for reducing varicocele symptoms. It is suggested to reduce the intake of caffeine and alcohol as long as the varicocele is not treated.
Does heavy lifting objects affect varicocele?
Yes, lifting, pushing, and pulling heavy objects for an extended period can form the varicocele and worsen its symptoms.
Can varicocelectomy treat azoospermia?
If the cause of azoospermia is varicocele disease, varicocelectomy can be treated. Through this surgery, people with azoospermia can increase their chance of producing healthy and motile sperm.












No reviews
Your comment