IVF Failure Reasons: Why Implantation Fails After IVF?
Fertility Treatment
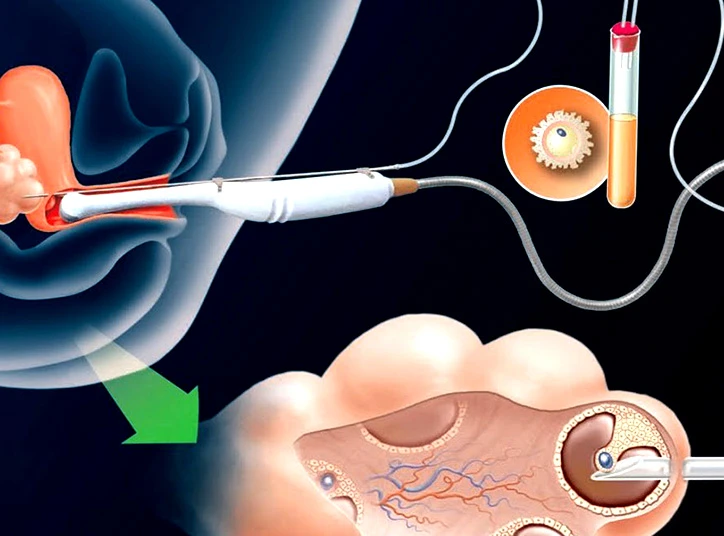
One of the most effective biotechnological methods in treating infertility is IVF treatment. The retrieved eggs and sperm are fertilized in the laboratory during this treatment, and the resulting embryo is transferred to the female partner's uterus. However, some couples may face IVF failure due to high maternal age, low egg quality, a problem in embryo development in the laboratory, implantation failure, etc. This article discusses IVF failure symptoms and causes of IVF failure with some techniques to lower its risk.

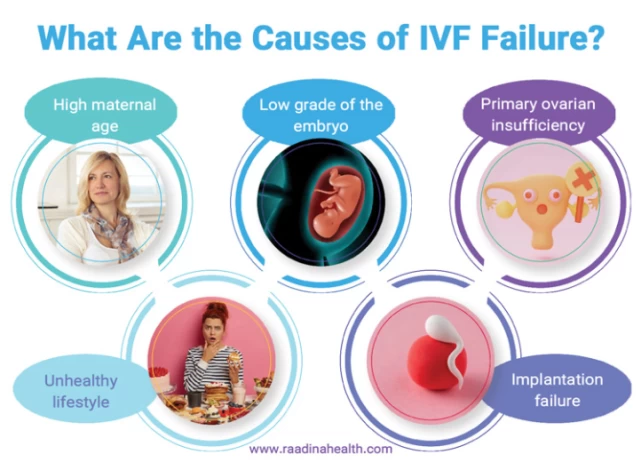
What Are the Causes of IVF Failure?
The success rate of IVF depends on many factors, including maternal age, cause of infertility, quality of sex cells and embryo, mother's BMI, couple's lifestyle, etc. IVF success is equal to this method's percentage of live births. In some cases, if the couple follows the specialist's instructions, the first cycle of IVF will be successful.
The following main causes of IVF failure are mentioned:
- High maternal age;
- Low grade of the embryo;
- Primary ovarian insufficiency (POI);
- Implantation failure;
- Uterine problems such as endometriosis;
- Unhealthy lifestyle;
- Chromosomal abnormalities.
In the following, we will introduce the IVF failure reasons mentioned items:
Role of Maternal Age in IVF Success
One of the most important IVF failure reasons for IVF is maternal age; the higher the mother's age, the lower the IVF success rate. Investigations have revealed that the success rate of IVF for 35-year-old women is about 32%, while this number decreases to 16% for women over 40.
In general, as the age of women increases, their ovarian reserve and their bodies' response to ovarian induction drugs decreases. Eggs retrieved from women over 40 are of low quality; as a result, the resulting embryos have a low grade. Moreover, women over 35 may face chromosomal disorders in the embryo, failure in the implantation, and abortion.

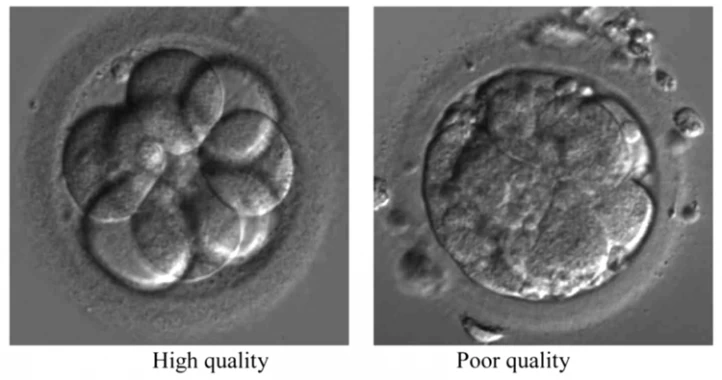
Quality of Embryo in IVF
The grade of the embryo depends on the quality of the sex cells. High-grade embryos can reach the blastocyst stage by 120 hours and stick to the endometrium easily. Different studies have shown that 79% of high-quality and 64% of good-quality embryos result in a live birth. Although the genomes of sex cells cannot be changed, the parents can improve the quality of their sperm and eggs by having a healthy lifestyle and a balanced diet.
Once again, the mother's age can affect the embryo's quality and IVF failure. Although one of four embryos fully develops during the IVF process, the chance of successful IVF in women 40 years old is almost 15%. One of the ways to overcome the problem of low egg quality is to use donor eggs from women under the age of 30, which increases the chance of IVF success despite the lack of genetic connection between the mother and the baby.
The embryo quality is also related to the quality of sperm. Factors such as sperm count, morphology, motility, and concentration are critical in having a high-grade embryo. Therefore, any deficiency in sperm parameters can lead to fertility problems and failure of assisted reproductive methods such as IVF, ICSI, or IUI.
Moreover, laboratory conditions for fetal development and precision and speed in the transfer process can significantly affect the embryo's quality to a great extent. Improper culture environment and a chromosomal disorder in the sex cells can also lead to implantation failure in 5 to 10 percent of cases. Therefore, if a chromosomal disorder is identified in the couple's DNA, they should take the PGD test (preimplantation genetic diagnosis) to lower the risk of passing on inherited diseases.
Primary Ovarian Insufficiency and IVF Failure
The female partner takes ovulation induction drugs in each IVF cycle to boost egg production. However, if she has primary ovarian insufficiency (POI), her body won't respond to IVF drugs, so that she won't produce enough mature eggs. Having low ovarian reserve and POI is one of IVF failure reasons.
Uterine Problems: The Main Causes of IVF Failure
A healthy uterus is one of the most important factors of IVF success. The doctor carefully examines the uterus using hysteroscopy and Doppler ultrasound for recurrent IVF failure. In hysteroscopy surgery, a special narrow camera called a hysteroscope examines all parts of the uterus and fallopian tubes. If there is any obstacle or problem in the female reproductive organs, the doctor resolves them before the start of the IVF procedure.
Implantation Failure in IVF
In IVF, the resulting embryo is transferred to the mother's womb after the fertilization phase, and the implantation process begins. IVF failure reasons such as ovarian cysts and polyps, uterine blood flow reduction, and anxiety after embryo transfer can increase the implant failure rate. In some cases, the development of the fetus stops before implantation; therefore, the uterus does not have any problem, and the cause of IVF failure is the embryo's low quality.
Unhealthy Lifestyles and Diet Lead to IVF Failure
To increase the chance of IVF success, you should have a healthy lifestyle before starting the treatment. Read on to learn what improves your sperm and egg parameters:
- Having vitamin supplements and folic acid;
- Drinking six to eight glasses of water a day;
- Having fresh fruit and vegetables, especially the ones with vitamins C and D;
- Having a healthy diet rich in fiber, protein, and minerals,
- Avoiding smoking;
- Maintaining a healthy BMI;
- Avoiding drinking alcohol and caffeinated beverages; and
- Exercising regularly.

Chromosomal Disorder: A Cause of IVF Failure
A chromosomal disorder in sex cells affects the quality of the embryo and causes IVF failure in many cases. In women over 35, the chromosomes in eggs are not divided correctly, so there wouldn't be 23 chromosomes in the egg.
The chromosomal abnormality in the sperm also affects the fetus's chromosomal structure and increases the risk of miscarriage. Usually, the male partner has a DNA problem in 15% of semen analyses with normal results. The DFI test can detect the rate of IVF failure in couples with DNA problems. Of course, there is no obligation to take the DFI test, but it has an important diagnostic role in finding the cause of infertility and repeated IVF failure. PGD test can also be used to check the health and chromosomal integrity of the embryo.
It should be noted that sometimes chromosomal disorders and genetic defects, the inability of the body to divide the cells and develop the embryo, the low grade of the embryo, and the rejection of the embryo by the mother's immune system cause implantation and IVF failure.
The disease that Causes Negative IVF
Blood clotting disorders in women can cause the embryo not to develop in IVF. In addition, some diseases, such as endometriosis, chronic fallopian tube infection, etc., can prevent implantation or development of the embryo and cause failure in IVF. Some of these factors include:
- Low Quality of Egg
- Low Ovarian Reserve
- Low Endometrial Receptivity
- The problem with Embryo Transfer
- The problem with Uterus or Fallopian Tubes
- Unbalanced TSH Level
- Blood Problems
- Infection
- Other Problems
Low Quality of Egg: Empty Follicle Syndrome (EFS)
In women with low egg quality, the follicles do not fully develop due to low ovarian reserve. Also, there would be some problems in retrieving mature eggs. Sometimes, even when the mother takes ovulation induction drugs and produces mature eggs, the eggs are considered "empty" due to their low quality. Pelvic adhesion and obstruction of the uterus by ovarian endometrioma may also cause the formation of empty eggs.

Low Ovarian Reserve
Excessive reduction in ovarian reserve can affect the success rate of IVF. IVF will probably be unsuccessful if the ovarian reserve is less than one. In such cases, the fertility specialist suggests using donor eggs.
Low Endometrial Receptivity
In case of having the following conditions, the receptivity of your uterus and your chance of IVF failure is low:
- Thin endometrial tissue;
- Uterine fibroids;
- Septate uterus;
- Intrauterine adhesions (IUAs);
- Uterus infection;
- Hydrosalpinx;
- Endometriosis, etc.
The problem with Embryo Transfer
Sometimes, the cause of IVF failure is the problems that happen during embryo transfer. Using the wrong catheter and tools or placing the embryo in the wrong place in the uterus will cause IVF to fail. On the other hand, by correcting the angle of the cervix and uterus, transferring the embryo by flexible and high-quality catheters, and using ultrasound during the transfer, the chance of successful IVF will increase.
The problem with Uterus or Fallopian Tubes
The condition of fallopian tubes is critical in IVF; if there is an obstruction in the fallopian tubes, they should be removed through salpingectomy before starting the treatment.
Since fallopian tube disorders lower the chance of IVF success, diagnosing and treating them are very important. Therefore, the following should be done before IVF:
- Diagnosing and treating hydrosalpinx (recurrent infection of the uterus);
- Identifying and removing obstruction or adhesions of the tubes;
- Performing laparoscopy to remove cervical lesions;
- Performing hysteroscopy surgery;
- Taking an ultrasound scan of the uterus and its vessels.
If you want more information about preparing the uterus for pregnancy, read this article.
Unbalanced TSH Level
A blood test to measure the level of TSH hormone and other hormones such as FSH, LH, and AMH helps check the possibility of miscarriage and diagnose the mother's thyroid problems.

Blood Problems
Blood clots and concentration can threaten the mother's life and increase the chance of miscarriage. Problems such as Hughes syndrome (also known as antiphospholipid syndrome and sticky blood) can be treated with blood thinners such as Clexane and a low dose of aspirin. Other blood problems that may affect IVF include thrombophilia, autoimmune diseases, etc.
Infection
Having an infection during IVF may lead to abortion. Infection can be diagnosed and treated by taking blood tests and antibiotics. Listeria and measles, infections caused by toxoplasmosis (transmissible through cat feces and unwashed fruits and vegetables), etc., are other factors that increase the risk of miscarriage.
Other Problems
Some other factors, such as lack of nutrients, anxiety, stress, uncontrolled diabetes, smoking, and exposure to pollutants and chemicals, also increase the rate of IVF failure.
What Does Repeated IVF Failure Mean?
It is perfectly normal to repeat the IVF cycle up to three times, but if it fails again after three unsuccessful attempts, the cause should be looked into. IVF failure can be attributed to two main factors: first, an issue with the embryo, and second, an issue with the couple. The primary reasons for repeated IVF failure are poor uterine health, low sperm and egg quality and quantity, poor embryo quality, and inappropriate embryo transfer. Even with high-quality embryos and a healthy uterus, if IVF fails more than three times, the doctor conducts additional tests to determine the reason.
How to Decrease the Risk of Miscarriage?
Some measures should be taken before and after IVF to decrease the risk of miscarriage, including:
- Taking hysteroscopy before IVF;
- Using appropriate progesterone after embryo transfer;
- Losing weight and maintaining a healthy BMI;
- Using a donor egg if the mother is over the age of 42;
- Avoiding heavy activities until the embryo is successfully implanted;
- Taking a blood test to identify thyroid problems and measuring AMH, FSH, and LH levels before IVF;
- Checking whether or not you have any infection;
- Examining blood problems such as blood concentration before the treatment.

Who Is Suitable for IVF?
Contrary to common belief, IVF is unsuitable for all infertile couples; people with the following features are considered ideal candidates for this treatment.
- Women with blockage or damage in one or both fallopian tubes;
- Men with low sperm count and low sperm motility;
- Women with ovulation problems;
- Women with uterine and ovarian disorders;
- People with genetic problems;
- People with unexplained infertility.
What Medications Interact with Fertility Drugs?
Taking some medications simultaneously with fertility drugs causes an imbalance in hormones and decreases their effect on the body. Therefore, before taking the following drugs, first consult your doctor:
- All medications, whether prescribed or OTC;
- Anti-allergy medications;
- OTC supplements;
- Ibuprofen (Advil) or acetaminophen (Tylenol)
It should be noted that doctors usually ask patients to stop taking the following drugs when starting IVF treatment:
- All types of steroids, such as asthma and lupus drugs;
- Non-steroidal anti-inflammatory drugs such as ibuprofen (Advil, Midol, Mortin), aspirin, and naproxen;
- Anticonvulsant drugs;
- Medicines to treat depression, anxiety, etc.
- Skin products containing estrogen or progesterone;
- Thyroid medication, and
- Chemotherapy drugs.
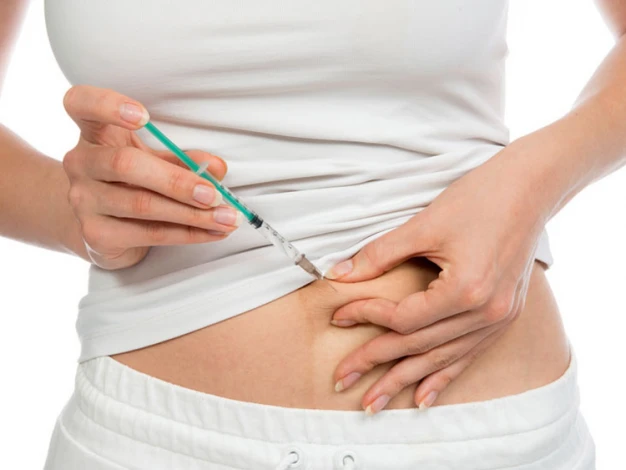
Is Bleeding After IVF Normal?
After an IVF transfer, light spotting and mild pain are perfectly normal; however, severe abdominal and pelvic pain and heavy bleeding are uncommon and may indicate an abortion. It should be noted that approximately 40% of women experience more bleeding during an IVF pregnancy than during a natural pregnancy.
Usually, the reason for bleeding is taking fertility drugs or vaginal examinations. Following embryo transfer, vaginal bleeding can be either light or heavy, and it can be either dark brown or light pink in color. Both successful and unsuccessful implantation can be indicated by spotting in the initial weeks following IVF, which can be treated with progesterone drugs. In any event, get in touch with your physician if you experience bleeding following an embryo transfer.
It is worth mentioning that it is impossible to confirm pregnancy and implantation based on the symptoms. The only definite way of confirming pregnancy is by taking a pregnancy test.
HCG Level After IVF
Two weeks after embryo transfer, the doctor asks you to take a blood or urine test to check the HCG hormone level in your blood. If you wonder whether HCG level indicates pregnancy after IVF, read on.
- If the amount of HCG hormone is less than 5 (mIU/mL), it is a sign of IVF failure.
- If the HCG level is more than 10 (mIU/mL), you should take the test 48 hours later to see if it doubles.
- If the hormone does not increase within 48 hours or its level decreases over time, the pregnancy may not last.
- If HCG increases significantly, the doctor performs an intravaginal ultrasound scan within four weeks after the transfer. In this case, the gestational sac will be filled with liquid and hold the embryo. A heartbeat should also be heard during the fourth to four and a half weeks after the transfer.

Factors that Increase IVF Success Rate
There are multiple methods to increase the IVF success rate, including:
- Scratching the endometrium;
- Injecting lymphocyte;
- Injecting platelet-rich plasma (PRP);
- Transferring embryo in the natural cycle;
- Using high-quality sperm;
- Hatching and removing the protective layer from the embryo to increase the chances of implantation;
- Investigating the genetic features of sex cells and embryos before transfer.
What to Do After IVF Failure?
After IVF failure, you should prepare your body and mind for repeating the cycle by considering the following tips:
- Stay positive and hopeful;
- Support each other and be patient;
- Take the necessary tests and fertility medications once more. You may need to inject 8 to 10 doses of drugs a day, but it is worth it;
- Cope with the side effects of fertility drugs, such as pain at the injection site, breast tenderness, nausea, headache, bloating, etc.;
- Ask a family member or friend to inject daily medications (if they know how to inject);
- Avoid hot baths, swimming pools, and saunas in the first days after repeated IVF cycle;
- Have a realistic expectation of the treatment's duration (2-3 weeks for ovulation stimulation, sperm retrieving, fertilization, and embryo transfer);
- Be mentally and physically prepared to repeat the IVF cycle if needed;
- Read more or ask your doctor about how many fertility shots you can take and how many times you can repeat ovarian puncture (3 to 6 times, depending on the condition of the ovaries);
- Read more about the success rate of IVF (usually 30-40%) to be mentally prepared for any outcome;
- You don't need bed rest between two IVF cycles, and you can do your daily activities as usual.

Success Rate of Second IVF Cycle
If the first IVF cycle fails, additional tests should be taken to investigate the cause of it. Therefore, failure in the first cycle of IVF does not reduce the chance of success in the following cycles. Repeating the IVF process can increase the chance of its success.
In the second IVF cycle, the success of the treatment depends on factors such as:
- the age of the mother,
- the quality of the sex cells,
- the doctor's skill in stimulating ovulation and transferring the embryo to the uterus,
- the causes of infertility,
- the condition of the uterus,
- the quality of the resulting embryos and
- the chromosomal and genetic characteristics of the embryo.
Couples who have experienced multiple unsuccessful IVF are recommended to change their doctor.
Increasing the Chance of Natural Pregnancy After Negative IVF
To increase the chance of a natural pregnancy after IVF, you can try the following:
- Reduce your weight and maintain a healthy BMI;
- Have a healthy diet rich in protein and vitamins;
- Stop smoking and drinking alcohol;
- Reduce caffeine intake and use prenatal vitamins;
- Pay extra attention to your ovulation and menstrual cycles;
- Control your stress by exercising and doing yoga;

As most fertility specialists suggest, assisted reproductive techniques should only be used if a couple cannot conceive naturally after six months of trying - in women over 35- or after one year of trying -in women under 35.
Successful IVF: Fertility Treatment in Iran
As mentioned earlier, multiple factors -such as maternal age, uterine condition, and embryo quality- affect the success rate of different fertility treatments, especially IVF. Another factor that has a high impact on the success of IVF is the skill and experience of the fertility doctor in diagnosing the cause of infertility and choosing the best treatment method for each couple.
As one of the main hubs in fertility treatment in the Middle East, Iran is an approved destination for couples despaired from repeating the IVF cycle. Iranian fertility specialists are experienced and adept in detecting the cause of infertility and eliminating it in the shortest time possible. Also, fertility clinics in Iran are equipped with the latest facilities and devices that can develop and keep the embryo at the highest quality for an adequate amount of time. In general, the success rate of IVF in Iran is more than 70%, which is relatively high compared to the nearby countries.




 WhatsApp
WhatsApp
 Telegram
Telegram
 Facebook
Facebook
 Email
Email














No reviews
Your comment